CASE STUDY 5
A Case Study by Dr. Naveen Tahasildar – Spine Surgeon in Bangalore
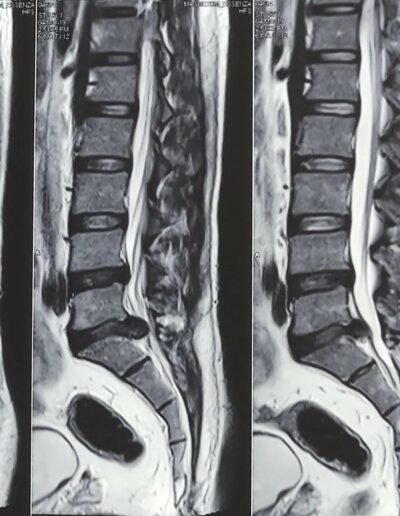
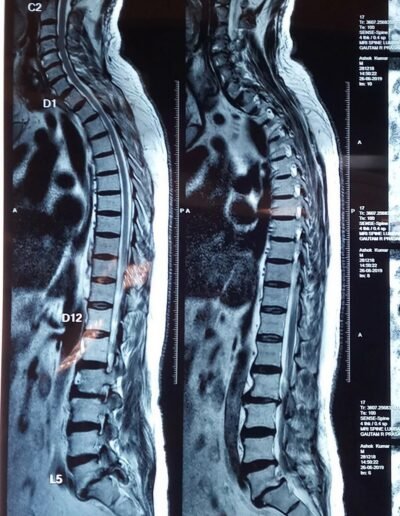
Mr. M, a 37-year-old IT professional, suffered from low back pain in the last 10 years which did not affect his activities of daily living significantly. However, his back pain increased in severity 3 months back following a heavy work. He also started having a radiating pain (sciatica) going down his left leg initially and then the right leg also. His MRI scans showed a L5-S1 disc prolapse which was compressing on the S1 nerve roots (these nerves travel down the leg to give power to the legs and carry sensation from the legs). This is one of the common scenarios that a spine surgeon handles on a day-to-day basis. A disc prolapse is an effect of wear and tear (degeneration) of discs, which are cushions between the vertebra (bricks which make a tower of spine to transfer weight of the body). The prolapsed disc irritates the nearby nerve root (inflammation). This is the primary reason for the radiating pain coming down the leg. This process lasts for about 2 to 3 weeks. The pain settles down as a natural process of healing in 90% of individuals. During this phase, we try to manage the pain to make the patient comfortable. The most common approach is to start simple anti-inflammatory medicines, a brief period of rest not more than 48 hours and lumbosacral corset (for 2 weeks only). It should be noted that these medicines don’t change the natural healing process but offer a quick relief to avoid prolonged suffering. In patients who do not respond to oral medicines, we give a nerve root block. This is a targeted injection of steroid and local anesthetic at the site of nerve root irritation under an x-ray guidance. This works instantly because the medications are delivered right at the site of problem. However, there are 10% of patients whose disc prolapse behaves differently in the following ways:
- The nerve root affected starts to lose its function which shows up as weakness of foot (commonly observed as a losing grip in the slippers) and increasing numbness or lost sensation.
- Even worse, some of them (<1%) start to develop numbness around the private parts and difficulty in voiding urine/loss of bladder control due to pressure on the major nerves.
- At the end of 3- 6 weeks, some of them persist to have radiating pain down the leg which compromises their quality of life significantly.
The first 2 categories are operated on an urgent basis to remove the pressure on nerve. The 3rd category (who are the most common) also require surgery on an elective basis to improve the quality of life. The surgery is called “Microdiscectomy”. A small keyhole is created in the back and under the microscope, the prolapsed disc is removed to make the nerve root free. The patient is made to walk after 3 hours of the surgery and discharged on the same next day. They can resume work by 2 weeks. Dr. Naveen Tahasildar – Consultant Spine Surgeon handled the case of patient Mr M. successfully by undergoing L5-S1 microdiscectomy because non-operative treatment tried for 3 months had not worked. He was discharged on the next day and has been able to go about his daily life with no problems.