Precise terminology helps healthcare professionals like spine specialists, communicate clearly about spinal anatomy, conditions, and interventions. For example, when describing spinal injuries or planning surgeries, knowing the exact vertebral level is crucial. This standardised nomenclature reduces confusion and enhances patient safety. Understanding the nomenclature for spinal regions can help patients better comprehend their diagnoses, treatments, and medical discussions related to spinal health.
The Five Main Spinal Regions
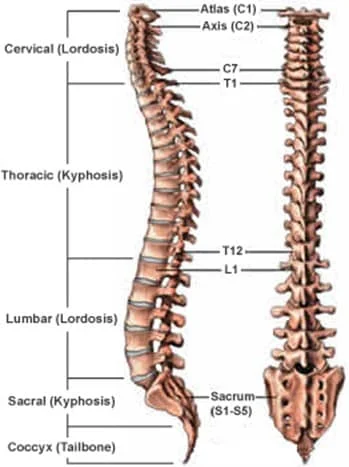
The human spine is divided into five distinct regions, each with a specific number of vertebrae and unique functions:
- Cervical Spine (Neck): Comprising 7 vertebrae (C1–C7), this region supports the head and allows for its wide range of motion.
- Thoracic Spine (Upper Back/Chest): Made up of 12 vertebrae (T1–T12), these vertebrae connect to the ribs and form part of the chest cage.
- Lumbar Spine (Lower Back): Consisting of 5 vertebrae (L1–L5), this region bears much of the body’s weight and provides flexibility and movement.
- Sacrum (Pelvic Region): Formed by 5 fused vertebrae (S1–S5), the sacrum connects the spine to the pelvis.
- Coccyx (Tailbone): Typically made up of 4 fused vertebrae, it is the lowest part of the spine.
Combined Spinal Regions in Clinical Practice
For certain medical purposes, adjacent spinal regions are considered together to describe conditions or procedures more precisely:
- Cervicothoracic Region: Combines cervical and thoracic vertebrae.
- Thoracolumbar Region: Combines thoracic and lumbar vertebrae.
- Lumbosacral Region: Combines lumbar and sacral vertebrae.
Advanced Nomenclature in Spinal Imaging and Procedures
In interventional spine medicine, a more detailed nomenclature system is used to describe specific anatomical zones within vertebral regions, especially during imaging and procedures such as injections or surgeries. These zones help clinicians report the exact location of pathology or treatment sites. For example, in the cervical spine, zones are divided into areas between key anatomical landmarks like the spinous processes and interlaminar spaces, aiding precision in interventions.
Surgical Nomenclature
- Procedure-Focused Terms: Surgeons often use nomenclature that describes the surgical approach, technique, and spinal segment involved. For example, in endoscopic spine surgery, standardized terms have been proposed such as:
- PECF: Posterior Endoscopic Cervical Foraminotomy
- TETD: Transforaminal Endoscopic Thoracic Discectomy
- TELD: Transforaminal Endoscopic Lumbar Discectomy
- IELD: Interlaminar Endoscopic Lumbar Discectomy
- LE-ULBD: Lumbar Endoscopic-Unilateral Laminotomy for Bilateral Decompression
These terms specify the approach (posterior, transforaminal, interlaminar), the spinal region (cervical, thoracic, lumbar), and the procedure performed (foraminotomy, discectomy, decompression).
- Histopathologic Descriptors: Surgeons may also use more detailed pathological terms based on tissue findings during surgery, which may not always match radiologic descriptions.
Pain and Functional Nomenclature
- Spine Cancer Pain: Standardized terminology includes biologic tumor pain, mechanical pain, radicular pain, neuropathic pain, and treatment-related pain, helping clinicians better identify and treat pain sources.
- Functional Units: Traditional naming of spinal interneurons by sensory input is being reconsidered in favor of functional classifications that reflect integrated motor behaviors.
Conclusion
Imaging specialties prioritize standardized, consensus-based terminology for clear communication of spinal findings, while surgical specialties use more detailed, procedure-oriented nomenclature to guide operative planning and documentation. These differences reflect the unique needs and goals of each specialty, but ongoing efforts to harmonize terminology can improve interdisciplinary collaboration.
For enquiries and online appointments:
Email – Naveen.st@gmail.com
Call/Whatsapp – +91 7676090119
Book/Schedule Appointment